It was the start of a busy day! A nurse told me that I would be seen be a physio who would get me walking. Walking? I didn’t know how to walk! I had completely forgotten how to walk. How was this possible? Whilst waiting for the physio, I remember fumbling on my phone, looking for videos on how to walk. I memorised the technique because I was terrified that not being able to walk would make me look silly. The physio arrived. Her name was Hannah and it would be the beginning of a beautiful friendship. She explained that ‘we’ would stand up and walk to the end of the bay, about 15ft. ‘Easy’ I said in a cocky way. Well – I couldn’t even stand, let alone walk. After many attempts at standing, under Hannah’s guidance, I was up! I was like a new born giraffe – shaking, legs going from under me and a sheer look of terror on my face. I put my trust in her and with her holding onto me, I took my first steps. She was very impressed with my technique!! I quickly became breathless and only managed 10ft, which felt like a marathon. She left me with lots of exercises to do and I was determined that by the next day, I would be up and down the corridor on my own!
After the positive start to the day, things quickly went downhill and I soon came to realise that being a long term patient in hospital was full of ups and downs. My temperature kept spiking and the liquid from my drains was a colour it wasn’t supposed to be. Suddenly, my mum and I were confronted by a doctor who we’d never met suggesting that I may have to be transferred to a different hospital in a different county. Fortunately, I was able to stay at Derriford but it caused unnecessary anxiety and confusion. The doctor was fluent in ‘medicalese’ and inflicted pure confusion onto myself and my family. I was later told that he shouldn’t have spoken to me without the consent of my consultant team. When a patient is in a fragile, confused state they need continuity and empathy from healthcare professionals and to be treated like humans.
However, in the afternoon, my faith was restored. I was told that the central line in my neck (a long thin tube that goes into the large vein near to the heart) would be removed but before doing so I would be having a ‘PICC’ line (similar to a central line but for longer use) inserted into my arm. I had no idea what to expect but I was chauffeured by bed down to what felt like the basement of the hospital and into a huge, clinical, cold room. There I met Ellen. At the time, Ellen was a student nurse on placement with the vascular team. I was still very weak and unable to move without help and had to attempt to move from my bed to the bed on which the procedure would take place. Ellen sprung into action, making sure that my diginity was preserved and her care and compassion immediately shone through. The surgeon explained what would happen, my anxiety went through the roof and the tears began! But with a little humour and kindness, I relaxed and the procedure began. I’ll never forget Ellen standing at the bottom of my bed, chatting to me about her nursing degree, what she hoped to do in the future and all the time distracting me from what was being done – very clever! The surgeon spoke to me as a human, not just another patient and he told me all about veins and pulses, showing me the ultrasound as it moved around my arm. It was quite fascinating.
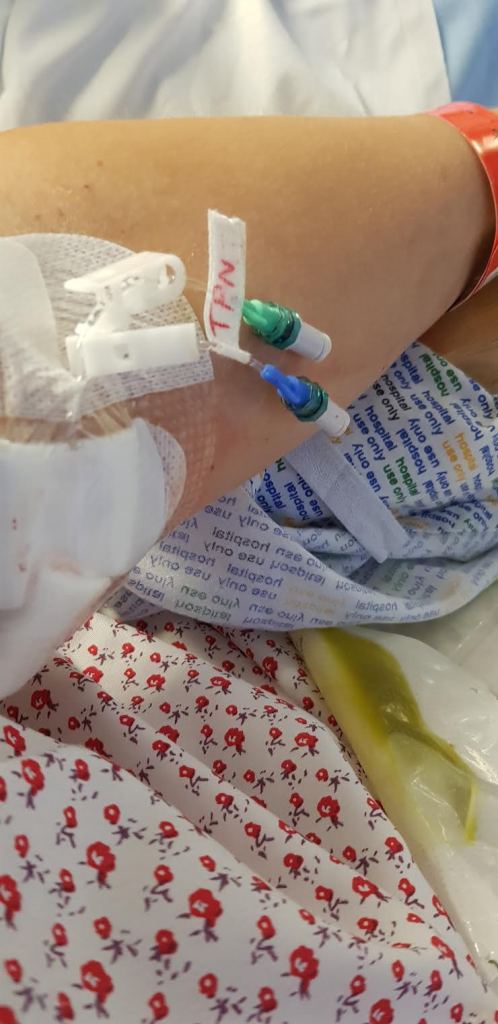
I returned to the ward and my central line was removed. It required me to lay still for quite some time as the line was close to my heart and time was needed for my body to settle. The nurse who carried out the procedure was Rachel and she became the first of many good ‘hospital friends’. She put me at ease and the line was out. It was another step forward, another step towards normality and another step towards the possibility of going home.
Ellen was wonderful and although I never got to meet her again, we follow each other on Twitter and I’m now thrilled to say that she’s a brilliant nurse. Thank you.

Leave a comment